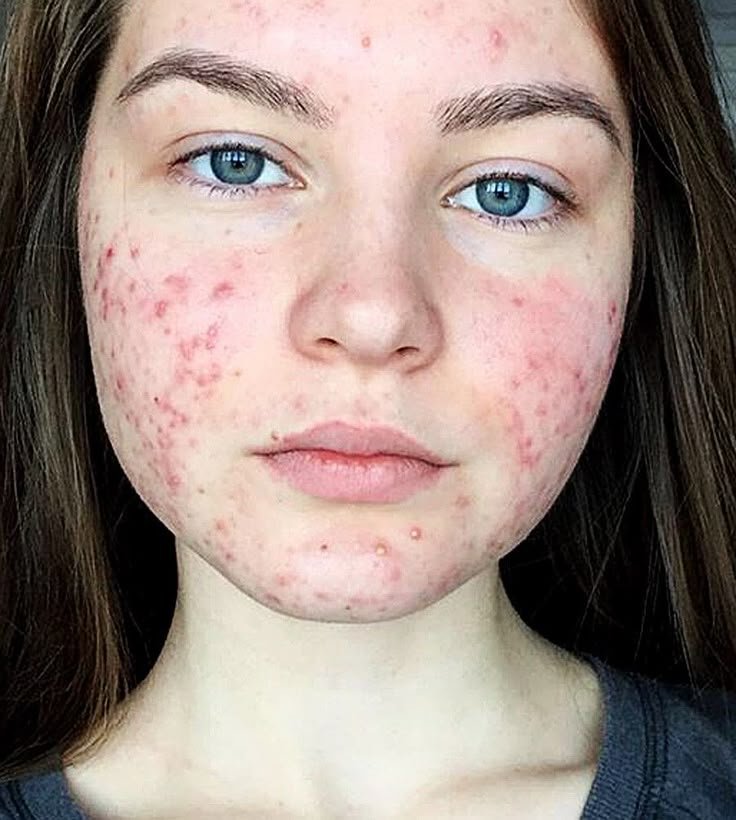
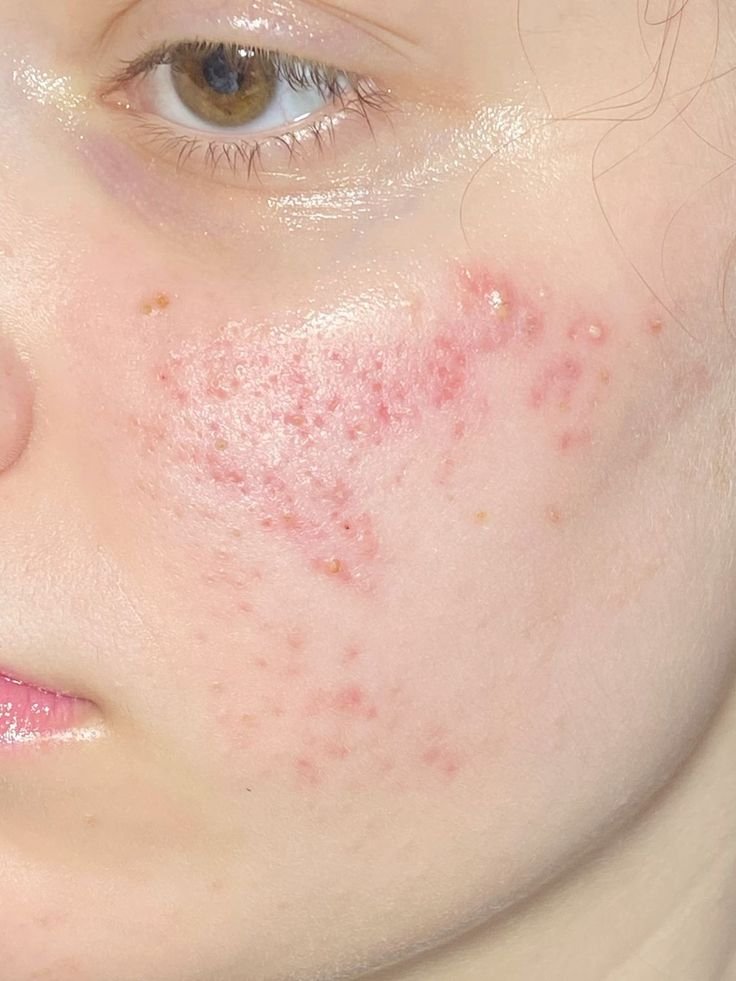
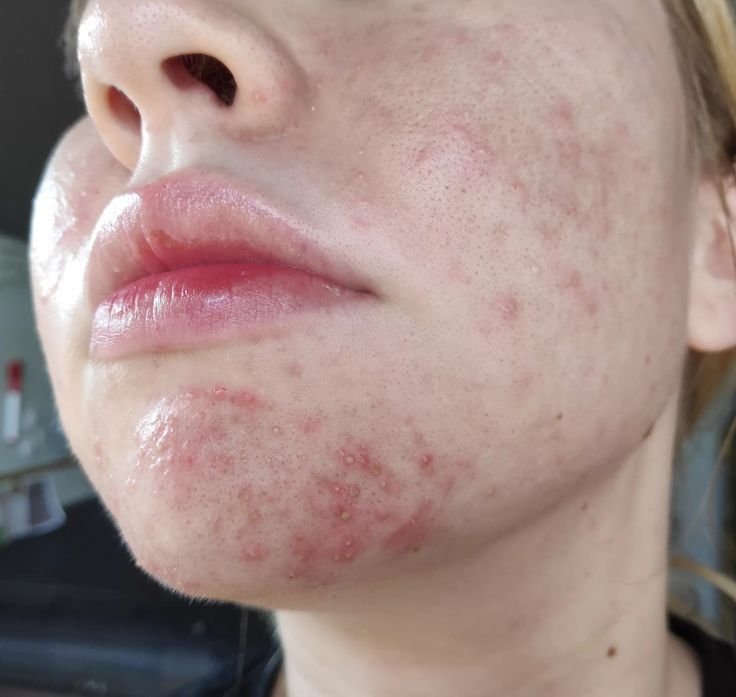
Acne Best Cure: Causes, Symptoms, Treatment, and Prevention Guide
Acne Best Cure is one of the most searched topics for anyone struggling with stubborn breakouts that refuse to respond to regular skincare routines. Many people spend months trying different creams, serums, and over-the-counter remedies, only to find minimal results, leaving them frustrated and confused. Understanding the causes, symptoms, and effective treatments for acne is essential for achieving clear and healthy skin. Acne can appear in different forms, from small pimples and whiteheads to cystic and inflamed lesions, and each type may require a different approach.
For effective acne Cure, it is important to first identify the underlying causes, such as hormonal imbalance, excess oil production, bacterial growth, or even lifestyle factors like diet and stress. Incorporating a proper skincare routine with gentle cleansers, non-comedogenic moisturizers, and targeted treatments can significantly reduce breakouts. Additionally, some people benefit from professional dermatological treatments, including topical antibiotics, retinoids, or chemical peels, depending on the severity of their acne.
Acne Best Cure with medical treatments, maintaining healthy habits like eating a balanced diet, drinking plenty of water, and avoiding heavy or oily skincare products can prevent future breakouts. By understanding the different aspects of acne best treatment, anyone can develop a personalized approach to achieve smoother, blemish-free skin. With A Acne Best Cure consistent care and the right guidance, clear and glowing skin is always achievable.
In this article, we’ll cover:
- What Acne pimples really is
- How it differs from regular acne
- The main causes and symptoms
- Effective treatment options (medical and natural)
- Prevention tips to avoid recurrence
By the end, you’ll be able to identify whether your breakouts are Fungal Bumps and know the best steps to achieve clear, healthy skin.
What is Acne?
acne, medically called Acne Vulgaris, is not a form of true acne. Instead, it’s caused by an overgrowth of Acne Best Cure that lives on the skin naturally. Normally, this yeast stays balanced with the skin’s bacteria, but when conditions change—like excess sweat, heat, or antibiotic use—it can multiply and infect hair follicles.
The result is red, uniform bumps that resemble acne but don’t respond to traditional acne products. That’s why so many people misdiagnose themselves and waste time on the wrong skincare solutions.
Key point:
- Regular acne = oil, dead skin, and bacteria clogging pores.
- Fungal skin breakout = yeast infection inside hair follicles.
How Fungal Acne Differs From Regular Acne
Because fungal acne looks similar, it’s easy to confuse it with bacterial acne. But there are important differences:
- Uniform bumps: All pimples are the same size and shape, unlike bacterial acne, where sizes vary.
- Clusters instead of random breakouts:Fungal Bumps often appears in patches or groups.
- Itchiness: A major clue. Malassezia folliculitis is itchy, while bacterial acne usually isn’t.
- Common areas: Forehead, chest, back, shoulders, and sometimes upper arms.
- Treatment resistance: Doesn’t respond to benzoyl peroxide, salicylic acid, or antibiotics.
👉 If you notice your breakouts are itchy, appear in groups, and don’t improve with regular acne products, you may be dealing with Malassezia skin infection.
Causes of Acne
There are several factors that can trigger or worsen Acne Best Cure. Understanding them helps with both treatment and prevention.
1. Excessive Sweat and Heat
Hot, humid climates create the perfect environment for yeast to thrive. People who sweat a lot—especially athletes—are more prone to Acne Best Cure.
2. Tight, Non-Breathable Clothing
Wearing synthetic fabrics during workouts or in hot weather traps sweat and heat against the skin, leading to fungal growth.
3. Overuse of Antibiotics
Antibiotics kill bacteria, but they don’t affect yeast. When good bacteria are reduced, yeast can grow unchecked, causing Fungal Folliculitis.
4. Oily Skincare and Hair Products
Since Malassezia yeast feeds on oil, heavy creams, body oils, and oil-rich shampoos can worsen Fungal Spots. “Sensitive skincare”
5. Weak Immune System
People with weakened immunity (due to illness, stress, or medication) are at higher risk of fungal infections.
6. Poor Hygiene Habits
Not showering after workouts, re-wearing sweaty clothes, or not washing pillowcases frequently can increase the chances of fungal breakouts.
Symptoms of pimples Acne
Recognizing symptoms is essential for diagnosis. Common signs include:
How to Confirm Fungal Acne
Dermatologists use skin scraping, biopsy, or lab tests to confirm Fungal-related pimple Acne.
But at home, you can strongly suspect it if:
Best Acne Cure
Because Acne Bumps isn’t bacterial, standard acne treatments won’t work. Instead, antifungal remedies are required.
1. Antifungal Cleansers
Use during showers 2–3 times a week:
- Ketoconazole shampoo (Nizoral) – apply as a face and body wash
- Selenium sulfide lotion/shampoo – reduces yeast growth
- Zinc pyrithione soap – antifungal cleansing option.
2. Topical Antifungal Creams
Over-the-counter creams that are effective:
- Clotrimazole cream
- Miconazole cream
- Ketoconazole cream
Apply a thin layer once or twice daily on affected areas.
3. Oral Antifungal Medications
For stubborn or widespread cases, dermatologists may prescribe:
- Fluconazole
- Itraconazole
These work internally to control fungal infections.
4. Skincare Routine Adjustments
- Use oil-free, non-comedogenic moisturizers
- Avoid coconut oil, olive oil, or shea butter
- Choose gel-based sunscreens instead of heavy creams
Home Remedies That May Support Treatment
Although not substitutes for medical care, some natural remedies may provide relief:
- Raw honey – antifungal and soothing
- Diluted tea tree oil – helps reduce yeast growth (must be diluted)
- Aloe vera gel – cools the skin, reduces redness, and itchiness
Prevention of Fungal Skin Rash
Because Yeast-induced Acne often comes back, prevention is as important as treatment.
- Shower immediately after sweating or workouts
- Wear loose, breathable fabrics like cotton
- Wash pillowcases, towels, and workout gear frequently
- Avoid heavy, oil-rich skincare products
- Maintain a balanced diet and reduce excess sugar (yeast feeds on sugar)
- Keep stress under control, since stress weakens immunity.

When to Seek Medical Help
See a dermatologist if:
- Your breakouts don’t improve with antifungal products
- Acne returns frequently
- The condition spreads to new areas
- You experience severe itching, discomfort, or inflammation.
FAQs About Fungal Acne
- Is fungal acne contagious?
No. It’s not contagious because it’s caused by yeast that naturally exists on your skin.
- Can Yeast-induced Acne go away on its own?
Mild cases may improve, but most require antifungal treatment to fully clear.
- Does diet affect Fungal Spots?
Yes. High sugar and carb-heavy diets can worsen Fungal Spots since yeast feeds on sugar.
- Do normal acne products help?
No. Benzoyl peroxide, salicylic acid, and antibiotics do not work against Pityrosporum Folliculitis Rash.
- Can fungal acne leave scars?
It usually doesn’t cause deep scars, but scratching can leave dark marks or hyperpigmentation.
Final Thoughts
Acne Best Cure can be frustrating because it looks just like regular acne, but the treatment is completely different.
- Identify Malassezia Breakouts by its itchy, uniform, and clustered bumps.
- Use antifungal cleansers and creams instead of standard acne products.
- Adjust your skincare to oil-free products and maintain good hygiene.
- Prevent recurrence with lifestyle changes like regular showers, breathable clothing, and a healthy diet. (healthline)
If your breakouts are stubborn and don’t respond to acne products, Acne Best Cure as the cause. With the right treatment and prevention steps, you can restore clear, healthy, and glowing skin.
For more information about acne, fungal acne, and the best skincare tips, follow our website regularly. Stay updated with expert advice and effective treatments to achieve clear and healthy skin.